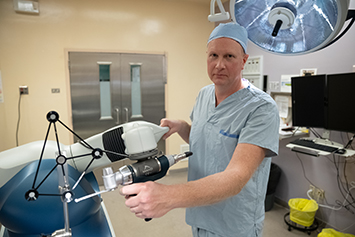
Innovating patient care with robotic-assisted surgery at Burnaby Hospital
Apr 17 2024
Retired Burnaby firefighter Jeff Clark spent years responding to emergencies and helping others. Decades of repeated use took a toll on his knees and when he needed surgery, Burnaby Hospital was there for him.
Media contact
For media inquiries, email media@fraserhealth.ca.
Tags
Media release
Surrey
High five your health care provider
New Westminster
Burnaby
Abbotsford
Langley
Maple Ridge
White Rock South Surrey
Chilliwack
Delta
Our People
Port Moody
Coquitlam
Humans of Fraser Health
Capital Project News
Mission
Pitt Meadows
Port Coquitlam
Awards
Our People
Development projects
Overdose
Seniors Nutrition
Program and services
Royal Columbian Hospital
Healthy eating
Hope
Seniors
Agassiz
Prevention
Long term care
Transform Surrey care
Physicians
Summer health
Navigation
nutrition
Burnaby Hospital
Child nutrition
Emergency department
Celebrating our people
Fraser Health
Mental health
Mental Health and Substance Use
Auxiliary
Burnaby development
Community
Health and wellness
Langley Memorial Hospital
The new Surrey hospital and BC Cancer Centre
Winter health
Heart to heart
New Westminster development
Back-to-school
Peace Arch Hospital
Surrey development
Volunteering
Abbotsford development
Baby and toddler nutrition
Capital Project Notice
Child immunizations
Peace Arch Hospital construction
Research
Surrey Memorial Hospital and community
Tools and technology
transforming
Baby and toddler oral health
Blog
Coronavirus
Flood response
Hospital
Hospitals
My workplace
Overdose response
Spring health
Transformation
Abbotsford Regional Hospital and Cancer Centre
Alcohol
Awards and recognition
Baby and toddler development
Breast milk donation
Burnaby Hospital redevelopment
Compassion
Eagle Ridge Hospital
Langley Memorial Hospital construction
Medical staff features
Pregnancy
Aboriginal Health
COVID-19
Child safety
Community Services
Emergency medicine
Harm reduction
Heart health
Hospice
Langley development
Measles
Metrotown Urgent and Primary Care Centre
Primary Care
Primary Care